In Vitro Fertilization (IVF) is a fertility treatment where eggs are fertilized outside the body and then transferred to the uterus. Learn how IVF works, who it’s for, success rates, and when it might be the right choice.
IVF (In Vitro Fertilization) is a fertility treatment where eggs are retrieved from the ovaries, fertilized with sperm in a lab, and the resulting embryo is transferred into the uterus to help achieve pregnancy.
IVF is one of the most effective and widely used forms of assisted reproductive technology (ART), offering a structured pathway to conception for individuals and couples facing fertility challenges. IVF is commonly used when other methods—such as ovulation induction or intrauterine insemination (IUI)—have not been successful or are not medically appropriate.
By combining precise hormonal stimulation, lab-based fertilization, and embryo transfer, IVF helps overcome various barriers to natural conception, including low egg count, blocked fallopian tubes, male infertility, or unexplained causes.
In this guide, you’ll learn how IVF works step-by-step, who it is recommended for, how long it takes, and what influences its success. Whether you’re at the beginning of your fertility journey or exploring advanced options, understanding IVF treatment is a crucial step toward making informed decisions.
Who Needs IVF?
IVF is recommended for individuals or couples who are unable to conceive naturally due to conditions like low ovarian reserve, blocked fallopian tubes, male infertility, or unexplained infertility.
In Vitro Fertilization (IVF) is not always the first step in fertility treatment, but it becomes a crucial option when simpler methods have failed or when medical conditions make natural conception unlikely. IVF allows doctors to bypass many of the natural barriers to fertilization and early embryo development.
Common reasons to consider IVF include:
- Low ovarian reserve or poor egg quality
As egg quantity and quality decline with age, especially after 35, IVF can help retrieve and use the healthiest remaining eggs—sometimes with additional techniques like ICSI or embryo freezing. - Blocked or damaged fallopian tubes
If eggs cannot travel from the ovaries to the uterus, natural conception is not possible. IVF bypasses the fallopian tubes entirely by fertilizing the eggs outside the body. - Endometriosis
Endometriosis can interfere with egg quality, fertilization, or implantation. IVF helps by controlling the entire process from egg retrieval to embryo transfer. - Male factor infertility
Low sperm count, poor motility, or abnormal sperm shape can make natural fertilization difficult. IVF with ICSI (Intracytoplasmic Sperm Injection) allows even a single healthy sperm to fertilize an egg. - Unexplained infertility
When no clear cause of infertility is found despite normal test results, IVF provides a direct route to conception and may reveal hidden factors during the process. - Genetic concerns or testing needs
Couples who carry inherited conditions may use IVF with preimplantation genetic testing (PGT) to screen embryos before transfer. - Recurrent pregnancy loss
IVF enables embryo monitoring and the option to test for chromosomal abnormalities, improving the chances of a successful pregnancy. - Fertility preservation
Individuals undergoing cancer treatment, or those who want to delay parenthood for personal or medical reasons, may freeze eggs or embryos via IVF for future use. - Same-sex couples or single parents
IVF supports family-building for people using donor sperm, donor eggs, or gestational carriers, depending on their reproductive needs.
The IVF Process Explained: Step by Step
IVF treatment involves a series of medical steps including ovarian stimulation, egg retrieval, fertilization in a lab, and embryo transfer into the uterus.
Each IVF cycle is carefully timed and monitored to maximize the chances of pregnancy. Here’s how a typical IVF process works:
1. Fertility Assessment and Planning
Before starting IVF, a complete fertility workup is done. This may include:
- Blood tests to check hormone levels (like AMH, FSH, LH, TSH, prolactin)
- Transvaginal ultrasound to evaluate ovarian reserve and uterine health
- Semen analysis for sperm count, motility, and morphology
- Review of medical history and past treatments
Based on this, the fertility specialist designs a personalised IVF plan.
2. Ovarian Stimulation
Goal: To produce multiple mature eggs in one cycle.
Daily hormone injections (FSH, HMG, or other gonadotropins) are given for 8–12 days to stimulate the ovaries. The growth of follicles is monitored via ultrasound and blood tests every few days.
When follicles are mature (usually 18–20 mm), a “trigger shot” (usually hCG or GnRH agonist) is given to prepare for egg retrieval.
3. Egg Retrieval (Ovum Pick-Up or OPU)
Timing: 34–36 hours after the trigger shot.
This is a short outpatient procedure done under mild sedation or anaesthesia. A needle is guided via ultrasound through the vaginal wall to retrieve eggs from the ovarian follicles.
The procedure takes about 15–20 minutes and most people resume normal activities the next day.
4. Sperm Collection and Preparation
Sperm is collected on the same day, either through ejaculation or (if needed) surgical retrieval. Donor sperm may also be used.
The sperm sample is “washed” and prepared in the lab to isolate the healthiest, most active sperm for fertilization.
5. Fertilization and Embryo Development
The retrieved eggs are combined with sperm in a lab. Two methods are used:
- Conventional IVF: Sperm and eggs are placed together in a culture dish and left to fertilize naturally.
- ICSI (Intracytoplasmic Sperm Injection): A single sperm is injected directly into each mature egg. ICSI is often used for male factor infertility or previous failed fertilizations.
The fertilized eggs (now embryos) are monitored over the next 3–5 days.
6. Embryo Selection and Transfer
Embryos are graded based on their appearance and development rate. On Day 3 or Day 5 (blastocyst stage), the best-quality embryo is selected for transfer.
Embryo transfer is a painless outpatient procedure where the embryo is gently placed into the uterus using a soft catheter. No anaesthesia is needed, and bed rest is not usually required.
Additional embryos (if any) can be frozen (cryopreserved) for future use.
7. Luteal Phase Support
After transfer, progesterone supplements (oral, injectable, or vaginal) are prescribed to support implantation and maintain the uterine lining.
8. Pregnancy Test and Follow-Up
About 10–14 days after embryo transfer, a beta hCG blood test is done to check for pregnancy. If the result is positive, early pregnancy monitoring begins.
If not successful, the next steps depend on how many frozen embryos are available, test results, and emotional readiness.
The IVF Timeline
A typical IVF cycle takes about 4 to 6 weeks, starting from ovarian stimulation to the final pregnancy test.
While the exact duration can vary slightly depending on your individual protocol and response to medications, here is a general timeline for one IVF cycle:
Day 1–2
Start of your menstrual cycle. Baseline tests and scans may be scheduled to confirm ovarian readiness.
Day 3–10
Ovarian stimulation begins. Daily hormone injections are administered to stimulate follicle growth. Ultrasounds and blood tests are done regularly to monitor progress.
Day 11–13
Final scans confirm follicle maturity. A trigger injection is given to prepare eggs for retrieval.
Day 13–15
Egg retrieval (OPU) is performed. On the same day, sperm is collected and fertilization is done in the lab.
Day 15–18
Embryo development is monitored. On Day 3 or Day 5, a viable embryo is selected for transfer.
Day 18–20
Embryo transfer is carried out. Progesterone support begins and continues until the pregnancy test.
Day 28–32
Blood test (beta hCG) is conducted to confirm pregnancy.
If there are frozen embryos, a Frozen Embryo Transfer (FET) cycle may be scheduled in a future month, which follows a shorter timeline as ovarian stimulation and retrieval are not repeated.
How IVF Success Is Measured
IVF success is measured by the ability to achieve a healthy pregnancy and live birth, with factors like age, egg and sperm quality, embryo grading, and uterine health playing key roles.
The success of an IVF cycle is not just about getting a positive pregnancy test—it’s about the full journey from embryo implantation to a live birth. Here’s how success is typically assessed, and what affects the chances of achieving it:
1. Age of the Person Providing the Eggs
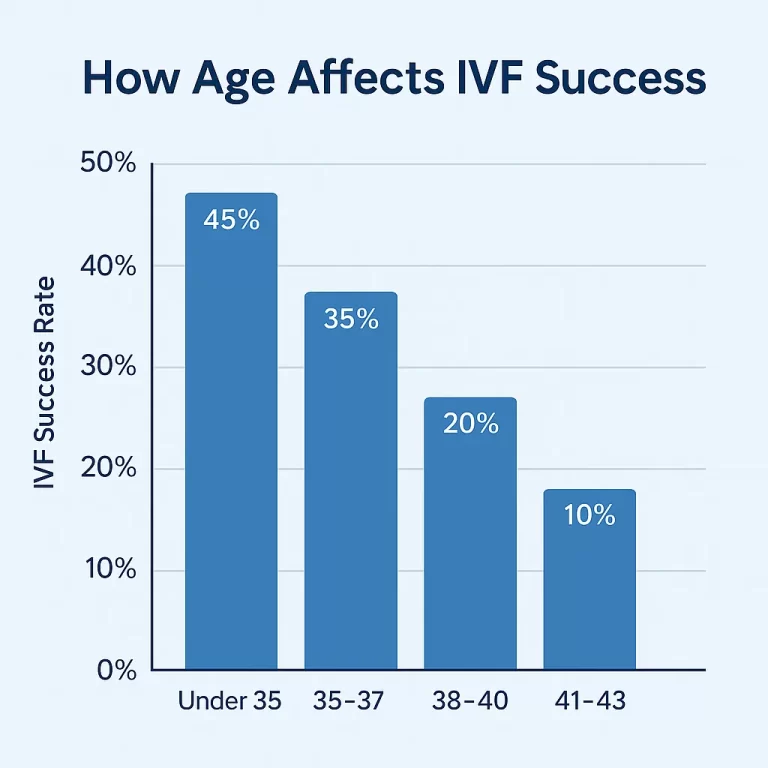
Age is one of the most important predictors of IVF success. Egg quality and quantity decline significantly after age 35, and more sharply after 40. Success rates for IVF using a person’s own eggs typically look like:
- Under 35: around 40–50% per cycle
- 35–37: around 30–40%
- 38–40: around 20–25%
- Over 40: less than 10–15%
If donor eggs are used, the success rate depends more on the donor’s age than the recipient’s.
2. Embryo Quality and Grading
Embryologists evaluate embryos based on their development and appearance. On Day 3, they are graded based on cell number and symmetry. On Day 5 (blastocyst stage), they are assessed for the inner cell mass and trophectoderm structure.
Higher-grade embryos are more likely to implant successfully, though even lower-grade embryos can sometimes lead to pregnancy.
3. Uterine Receptivity and Lining Thickness
A healthy uterine lining is critical for successful implantation. Ideally, the endometrial thickness should be around 8–12 mm at the time of transfer. Hormone levels and the timing of the transfer also influence uterine receptivity.
Some clinics offer an ERA (Endometrial Receptivity Array) test to personalise the timing of embryo transfer for optimal results.
4. Sperm Quality
Male fertility factors such as low sperm count, poor motility, or abnormal morphology can affect fertilization and embryo development. Techniques like ICSI (Intracytoplasmic Sperm Injection) are used in such cases to improve outcomes.
5. Number of Embryos Transferred
Transferring more than one embryo may increase the chance of pregnancy, but also raises the risk of multiple births. Many clinics now prefer single embryo transfer (SET) with high-quality blastocysts to reduce risks and improve maternal outcomes.
6. Use of Additional Technologies
Advanced lab techniques may improve outcomes in certain cases:
- ICSI helps when sperm factors are an issue
- PGT-A (Preimplantation Genetic Testing for Aneuploidy) screens embryos for chromosomal abnormalities
- Time-lapse embryo monitoring helps select the most viable embryos without disturbing development
- Assisted hatching can be used in selected cases to improve implantation potential
7. Lifestyle and Health Factors
Body weight (BMI), smoking, alcohol intake, stress, thyroid function, and chronic conditions like PCOS or diabetes can all influence success rates. Addressing these through pre-IVF counseling or lifestyle changes can improve outcomes.
8. Cumulative Success Across Multiple Cycles
While a single cycle may not always be successful, many people achieve pregnancy over multiple IVF attempts. Cumulative success rates increase with each high-quality cycle, especially when frozen embryos are available for transfer without repeating stimulation.
Tracking IVF success is a multi-dimensional process. The goal isn’t just a pregnancy test—it’s a healthy birth. Understanding these factors can help manage expectations and prepare emotionally and medically for the journey.
Risks and Side Effects of IVF
IVF is generally considered safe, but it can involve physical, emotional, and financial risks—including medication side effects, multiple pregnancy risk, emotional stress, and occasional complications during the cycle.
While millions of IVF cycles are performed safely each year, it’s important to be aware of the potential side effects and risks involved so you can make informed decisions and prepare accordingly.
1. Ovarian Hyperstimulation Syndrome (OHSS)
OHSS is a condition that may occur when the ovaries over-respond to fertility medications. It can cause:
- Abdominal bloating
- Nausea or vomiting
- Sudden weight gain
- Pain or fluid buildup in the abdomen
Mild OHSS is relatively common and resolves on its own. Moderate to severe cases are less frequent but may require close monitoring or temporary hospital care. Modern protocols and trigger medication adjustments have significantly reduced its incidence.
2. Multiple Pregnancy
Transferring more than one embryo increases the risk of twins or higher-order multiples. While some may see this as a positive outcome, multiple pregnancies carry higher risks of:
- Preterm labor and low birth weight
- Gestational diabetes
- Preeclampsia and delivery complications
- Neonatal intensive care admission
To reduce this risk, many clinics now follow single embryo transfer (SET) guidelines, especially for younger patients or those using genetically tested embryos.
3. Egg Retrieval Procedure Risks
Though generally safe, egg retrieval is a minor surgical procedure and carries small risks such as:
- Bleeding
- Infection
- Reactions to sedation
- Ovarian or pelvic discomfort after the procedure
These are rare and usually managed effectively with routine precautions.
4. Ectopic Pregnancy
In rare cases, the embryo may implant outside the uterus, usually in the fallopian tube. This is called an ectopic pregnancy and requires immediate medical attention. The rate of ectopic pregnancy in IVF is low, typically between 1–2%.
5. Emotional and Psychological Impact
IVF can be emotionally demanding. The combination of hormone injections, time-sensitive procedures, financial cost, and uncertainty can contribute to:
- Mood swings or emotional fatigue
- Anxiety and disappointment after a failed cycle
- Pressure from repeated cycles or social expectations
Having emotional support, fertility counseling, or access to a peer support group can help reduce psychological strain throughout the process.
6. Medication Side Effects
Hormone injections used during ovarian stimulation may cause temporary side effects such as:
- Bloating
- Breast tenderness
- Headaches
- Irritability
- Mood changes
These typically subside after the retrieval phase or when hormone levels stabilize.
7. Long-Term Health Concerns
Current research shows no significant long-term health risks for most people who undergo IVF. However, ongoing studies continue to monitor associations between IVF and conditions like ovarian cancer, though no direct causal link has been established with modern stimulation protocols.
Understanding both the benefits and the potential drawbacks of IVF helps patients feel more prepared and less overwhelmed. Open conversations with fertility specialists and proactive care planning are key to managing these risks effectively.
Cost of IVF Treatment in India
The cost of one IVF cycle in India typically ranges between ₹90,000 and ₹2,50,000, depending on the clinic, treatment protocol, medications, and whether additional procedures like ICSI, embryo freezing, or donor support are required.
India is one of the most cost-effective countries for IVF globally, offering high-quality treatment at a fraction of the cost in Western countries. However, prices can vary based on location, medical complexity, and the technologies involved.
What’s Usually Included in the Base IVF Cost
A standard IVF package may include:
- Initial consultation and basic fertility tests
- Ovarian stimulation injections
- Follicular monitoring (ultrasounds and hormone tests)
- Egg retrieval and sedation
- Sperm processing
- Fertilization (conventional IVF)
- Embryo culture for 3–5 days
- Fresh embryo transfer
- Pregnancy (beta hCG) test
In most cases, medications are billed separately and can cost ₹50,000–₹80,000 depending on your dosage and protocol.
What May Cost Extra
The following are typically not part of the basic IVF package and are charged additionally:
- ICSI (Intracytoplasmic Sperm Injection): ₹20,000–₹50,000
- Embryo freezing (vitrification): ₹20,000–₹35,000
- Storage of frozen embryos: ₹5,000–₹15,000 per year
- Frozen embryo transfer (FET): ₹30,000–₹60,000
- Preimplantation Genetic Testing (PGT-A): ₹60,000–₹1,50,000
- Donor egg/sperm services: ₹30,000–₹70,000 depending on source
Factors That Influence IVF Cost
- Location of the clinic (metro cities like Delhi, Mumbai, Bangalore usually have higher costs but better facilities)
- Experience and success rate of the fertility center
- Patient’s age and ovarian reserve (affects medication dose and protocol)
- Need for additional treatments like IUI, laparoscopy, or hysteroscopy prior to IVF
- Use of donor gametes or gestational carriers
Can You Get IVF Under EMI or Insurance?
Most health insurance plans in India do not cover IVF, although some newer plans now include it as an add-on. Many fertility clinics offer EMI or financing options to make treatment more accessible.
It’s important to ask for a transparent cost breakdown before starting treatment and clarify what’s included in any package offered.

Myths and Facts About IVF
Despite being a medically advanced fertility treatment, IVF is surrounded by myths that can cause confusion, fear, or unrealistic expectations. Separating facts from misinformation helps people make informed decisions about their reproductive health.
Here are some of the most common IVF myths—and the truth behind them:
Myth 1: IVF guarantees a pregnancy
Fact:
IVF offers one of the highest success rates among fertility treatments, but it cannot guarantee pregnancy. Success depends on many factors—like age, egg and sperm quality, uterine health, and embryo viability. Even under ideal conditions, IVF success per cycle can range from 30% to 50% for younger individuals.
Myth 2: IVF is only for older women
Fact:
While IVF is often recommended for those over 35 due to age-related fertility decline, it is also used by younger people facing conditions like endometriosis, PCOS, low sperm count, blocked tubes, or unexplained infertility. In fact, success rates are usually higher in younger age groups.
Myth 3: IVF often results in twins or triplets
Fact:
Modern IVF protocols aim for single embryo transfer (SET) to avoid the risks of multiple pregnancies. Clinics now carefully select one healthy embryo for transfer, and twins are less common than they used to be.
Myth 4: IVF babies are weak or “unnatural”
Fact:
IVF babies are just as healthy and normal as those conceived naturally. The method of conception has no negative impact on intelligence, health, or emotional development. IVF simply helps where nature struggles.
Myth 5: IVF is always too expensive
Fact:
IVF in India is more affordable than in many parts of the world. While not cheap, many clinics offer structured packages, EMI plans, and transparent pricing. Costs also vary depending on whether you need additional procedures like ICSI or embryo freezing.
Myth 6: You need to rest completely after IVF
Fact:
Routine activities like walking, working, or light exercise are generally safe after embryo transfer. Complete bed rest is not required unless advised by your doctor for specific reasons. Staying mentally relaxed often matters more than physical restrictions.
Myth 7: IVF is your only option if you can’t conceive
Fact:
IVF is just one of several fertility treatments. Options like ovulation induction, IUI, lifestyle changes, or surgical correction of certain conditions may work depending on the case. IVF is usually recommended when these approaches have failed or are unlikely to succeed.
By understanding what IVF can and cannot do, individuals can approach treatment with realistic expectations and less anxiety.
FAQs About IVF Treatment
If you’re considering IVF, it’s natural to have questions—about the process, the risks, the results, and what daily life looks like during treatment. This section answers some of the most common concerns people have before beginning IVF, so you can move forward with more clarity and confidence.
1. Is IVF painful?
IVF is not typically painful. Most people find hormone injections manageable, and egg retrieval is done under anaesthesia or sedation. Some mild cramping or bloating can occur during the stimulation or after the retrieval, but the overall discomfort is minimal and temporary.
2. Can I work during IVF treatment?
Yes, most people continue working throughout the IVF cycle. Monitoring appointments may require some flexibility, and you may want to rest for a day after the egg retrieval and embryo transfer, but no extended downtime is required.
3. How many embryos are transferred during IVF?
Usually, one embryo is transferred to reduce the risk of multiple pregnancy. In some cases, especially for older patients or after previous failed cycles, two embryos may be considered. The decision is made based on embryo quality and clinical history.
4. Can IVF be done using donor eggs or sperm?
Yes. IVF can be performed using donor sperm, donor eggs, or even donor embryos, depending on your fertility condition or personal circumstances. Donor options are commonly used in cases of poor egg quality, azoospermia, or genetic concerns.
5. What happens to extra embryos?
Good-quality extra embryos can be frozen (vitrified) and stored for future use. Frozen embryo transfers (FET) can be done later without repeating the full IVF cycle.
6. Is bed rest necessary after embryo transfer?
No, extended bed rest is not required. Light activity is generally safe. Some people prefer to rest for a few hours after transfer, but there’s no evidence that lying down improves success rates.
7. How soon will I know if IVF has worked?
A beta hCG blood test is usually scheduled 10 to 14 days after the embryo transfer to confirm pregnancy. Urine pregnancy tests are not recommended during this period as they may show misleading results due to lingering hormones.
8. Can IVF be repeated if it fails?
Yes. Many people go through more than one IVF cycle. Doctors typically adjust protocols based on your response to previous cycles, and frozen embryos can often be used for subsequent attempts without starting from scratch.
9. Are IVF babies different from naturally conceived babies?
No. IVF babies are just as healthy and normal as those conceived naturally. Studies have shown no difference in terms of physical health, mental development, or emotional well-being.
10. Is IVF safe in the long run?
Current research shows that IVF is generally safe for both the person undergoing treatment and the child. Like any medical procedure, there are risks, but serious long-term complications are rare.
Is IVF Right for You?
IVF is a scientifically proven and widely practiced fertility treatment that offers hope and results for many individuals and couples struggling to conceive.
By combining controlled hormonal stimulation, lab-based fertilization, and precise embryo transfer, IVF helps overcome many reproductive challenges that natural conception cannot. While it doesn’t guarantee pregnancy, it remains one of the most effective options available—especially when guided by timely diagnosis and personalised care.
Understanding how IVF works, who it’s for, and what influences success can help you make confident, well-informed decisions about your next steps. Whether you’re at the start of your fertility journey or exploring treatment after other methods, IVF is a path worth considering with the right medical support.





