Assisted Reproductive Technology (ART) refers to a group of medical treatments that help individuals or couples conceive by directly handling eggs, sperm, or embryos in a controlled laboratory setting.ART is most often used when natural conception is not possible or has repeatedly failed, offering a scientifically backed route to pregnancy through methods such as in …
Assisted Reproductive Technology (ART) refers to a group of medical treatments that help individuals or couples conceive by directly handling eggs, sperm, or embryos in a controlled laboratory setting.
ART is most often used when natural conception is not possible or has repeatedly failed, offering a scientifically backed route to pregnancy through methods such as in vitro fertilization (IVF), intracytoplasmic sperm injection (ICSI), intrauterine insemination (IUI), and the use of donor gametes or embryos. It also includes more complex procedures like embryo freezing, genetic testing, and gestational surrogacy.
In simple terms, ART bridges the gap between biological barriers and parenthood by replicating or supporting the process of fertilization and implantation outside the body. These treatments are designed to support people with infertility, same-sex couples, and individuals who need fertility preservation due to medical or personal reasons.
The use of ART has grown significantly across the world in the last few decades, not only because of rising infertility rates but also due to greater awareness, improved technology, and expanded access to treatment. In India alone, ART has become one of the most accessible and sought-after categories of fertility care, thanks to a large network of clinics, experienced embryologists, and comparatively lower costs than in countries like the US, UK, or Australia.
Despite its increasing popularity, ART remains a complex field involving both medical precision and deeply personal choices. Understanding what ART really means—and how it works—can help people feel more confident in exploring their fertility options.
ART is not a single treatment, but a spectrum of techniques. Some of the most commonly used procedures under ART include:
- In Vitro Fertilization (IVF): Fertilization of eggs and sperm outside the body, with embryo transfer into the uterus.
- Intracytoplasmic Sperm Injection (ICSI): Injection of a single sperm directly into an egg, used for severe male infertility.
- Intrauterine Insemination (IUI): Processed sperm is placed directly into the uterus during ovulation to increase chances of fertilization.
- Egg or Sperm Donation: Used when one partner’s gametes are not viable or in donor-conception cases.
- Embryo Freezing (Cryopreservation): Preserves embryos for future use, especially useful in case of surplus or for fertility preservation.
- Preimplantation Genetic Testing (PGT): Screening embryos for chromosomal or genetic conditions before transfer.
- Gestational Surrogacy: An embryo is implanted into a surrogate who carries the pregnancy for another individual or couple.
The level of complexity, cost, and intervention varies depending on the method chosen and the reasons for using it.
It’s also important to distinguish ART from more basic fertility treatments. For example, ovulation induction with medication or lifestyle changes to improve hormonal balance are not considered ART. The defining feature of ART is the handling of eggs and sperm outside the human body, typically in a lab setting, which marks a more advanced stage of intervention.
Over time, the term ART has come to represent not just a medical toolkit but also a shift in reproductive possibilities. It empowers individuals—whether single, partnered, older, LGBTQIA+, or facing medical challenges—to have biological children using personalized and science-based support.
As ART continues to evolve, it raises important conversations about ethics, access, and the future of reproductive health. But at its core, ART is about creating opportunities where nature may be limited—giving people a safe, structured, and clinically supported path to building the families they want.
Why Is Assisted Reproductive Technology (ART) Used?
Assisted Reproductive Technology is used when natural conception is not possible, not advisable, or has repeatedly failed despite other medical interventions. While the reasons for choosing ART can vary widely, the goal is always the same: to improve the chances of a healthy, viable pregnancy by medically assisting key stages of fertilization, embryo development, and implantation.
For many individuals and couples, ART offers a pathway forward after months or years of uncertainty. It becomes an option not only when infertility has been diagnosed, but also when medical, personal, or genetic circumstances require more controlled and precise methods of conception.
ART is often used in the following scenarios:
- Blocked, damaged, or absent fallopian tubes
If the fallopian tubes are not functional or have been removed, natural fertilization cannot occur. IVF bypasses the tubes entirely by fertilizing the egg in a lab. - Male factor infertility
Issues such as low sperm count, poor motility, or abnormal sperm morphology can prevent fertilization. ICSI allows direct injection of a healthy sperm into the egg, significantly improving outcomes in such cases. - Advanced maternal age or diminished ovarian reserve
As fertility declines with age—especially after 35—ART can help retrieve and use the best available eggs and allow for embryo freezing or genetic screening. - Unexplained infertility
When all tests appear normal but pregnancy still does not occur, ART can offer a more controlled environment to identify potential issues and improve the likelihood of success. - Endometriosis and other pelvic disorders
Conditions like endometriosis, fibroids, or adhesions may interfere with the normal function of reproductive organs. ART helps bypass these physical barriers to conception. - Repeated miscarriages or implantation failure
For individuals who conceive but cannot carry a pregnancy to term, ART allows for embryo selection, genetic testing, and advanced support to improve outcomes. - Same-sex couples and single parents
ART provides access to family-building options for LGBTQIA+ individuals and single people through the use of donor sperm, donor eggs, or gestational surrogacy. - Fertility preservation before medical treatment
People undergoing cancer treatment, surgery, or gender-affirming procedures may choose to preserve eggs, sperm, or embryos in advance, to use later through ART. - Genetic conditions in either partner
ART allows for preimplantation genetic testing (PGT) to identify embryos that are chromosomally normal or free of inherited disorders before implantation.
Beyond clinical need, ART also serves those who wish to plan their families with more control—whether that means delaying parenthood, avoiding specific health risks, or growing a family in non-traditional ways.
It is not just a response to infertility—it is a modern tool that expands reproductive choice. As awareness increases and social norms evolve, ART is playing a growing role in supporting diverse paths to parenthood.
Types of Assisted Reproductive Technology (ART)
Assisted Reproductive Technology includes a wide range of medical procedures designed to support or enable conception by working with eggs, sperm, and embryos outside the body. The choice of technique depends on the cause of infertility, the age and reproductive history of the individuals involved, and their specific medical or personal circumstances.
While IVF is the most well-known ART procedure, there are several others that serve different needs at different stages of the reproductive process. Some are used alone, while others are often combined to improve success rates or tailor treatment.
Here are the major types of ART used in clinical practice today:
- In Vitro Fertilization (IVF)
IVF involves retrieving mature eggs from the ovaries, fertilizing them with sperm in a lab, and transferring the resulting embryo(s) into the uterus. It is one of the most widely used and effective ART procedures and is often recommended when other methods have failed or are not applicable. - Intracytoplasmic Sperm Injection (ICSI)
ICSI is a specialised form of IVF used primarily in cases of male factor infertility. Instead of combining sperm and egg in a dish, a single healthy sperm is injected directly into a mature egg to ensure fertilization. - Intrauterine Insemination (IUI)
IUI is sometimes included in discussions of ART, though it does not involve handling of eggs or embryos in a lab. Sperm is washed and directly introduced into the uterus during ovulation, making it easier for fertilization to occur naturally. - Donor Egg and Donor Sperm Programs
When one partner cannot provide viable eggs or sperm, donor programs offer a solution. Eggs or sperm from a healthy donor are used for fertilization via IVF or IUI. This is common in cases of advanced maternal age, premature ovarian insufficiency, or azoospermia. - Embryo Donation
In some cases, surplus embryos from another couple’s IVF cycle are donated to individuals or couples who are unable to conceive with their own gametes. This option is legally and ethically regulated, and typically involves anonymous donation. - Gestational Surrogacy
A surrogate (gestational carrier) carries and delivers a baby for another individual or couple. The embryo is created using the intended parent(s)’ sperm and/or egg (or donor gametes) and is implanted into the surrogate’s uterus. This is often used in cases of uterine absence or repeated pregnancy loss. - Fertility Preservation (Cryopreservation)
Eggs, sperm, or embryos can be frozen for future use. This is recommended for individuals undergoing medical treatments (like chemotherapy), or those who wish to delay childbearing for personal or professional reasons. - Preimplantation Genetic Testing (PGT)
PGT involves screening embryos for chromosomal abnormalities (PGT-A) or specific genetic conditions (PGT-M, PGT-SR) before implantation. It helps reduce the risk of miscarriage or inherited disorders, especially in high-risk cases.
Each of these technologies offers unique benefits and may be used individually or in combination depending on the case. For example, IVF with ICSI and PGT is common in cases of male infertility and repeated IVF failure, while egg freezing followed by IVF is often used for fertility preservation.
Understanding the available options is a critical step in choosing the right course of treatment. The next section will walk through how ART procedures typically unfold—what to expect before, during, and after treatment.
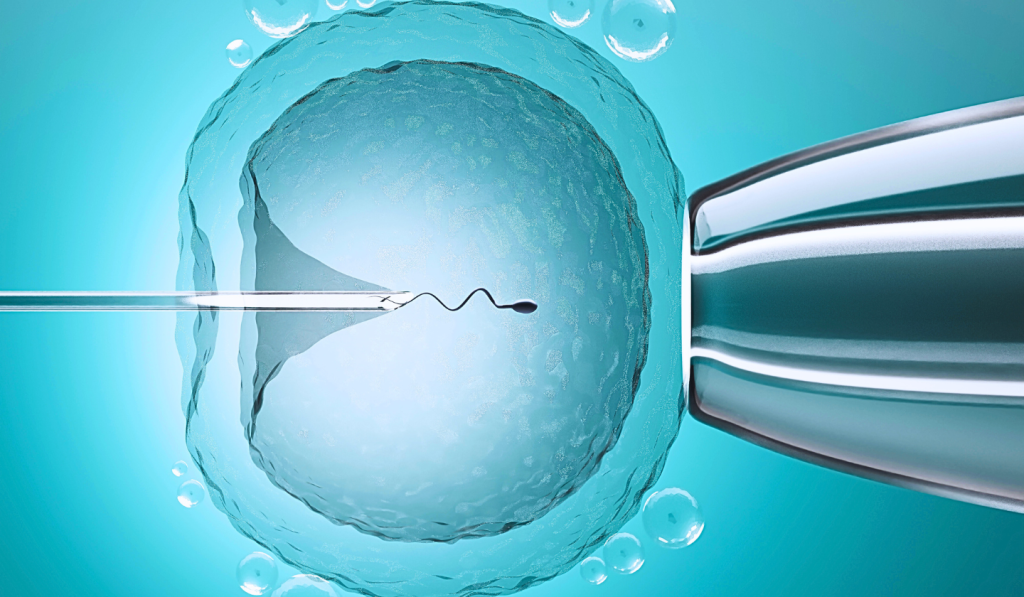
How Assisted Reproductive Technology (ART) Works – Step by Step
Assisted Reproductive Technology involves multiple stages, carefully timed and medically supervised, to maximise the chances of successful conception and implantation. While each ART method may follow a slightly different course, most procedures—especially IVF and related treatments—follow a general structure built around the key phases of testing, stimulation, fertilization, and embryo transfer.
This section outlines the typical journey through an ART cycle, with a focus on what happens at each step and what patients can expect along the way.
Initial Assessment and Fertility Workup
Before starting ART, a complete fertility evaluation is done to understand the underlying issues and decide which treatment is best suited. This may include:
- Hormonal blood tests (like AMH, FSH, LH, TSH, prolactin)
- Ultrasound scans to assess ovarian reserve and uterine health
- Semen analysis to evaluate sperm count and motility
- Infection screening and overall health assessment
The fertility team uses this information to design a personalised protocol that addresses your specific diagnosis and reproductive goals.
Ovarian Stimulation
For procedures like IVF and ICSI, hormone injections are used to stimulate the ovaries to produce multiple eggs. This phase typically lasts 8 to 12 days, during which follicle growth is closely monitored through ultrasounds and blood tests.
The goal is to retrieve more than one mature egg to improve fertilization chances and allow for embryo selection or freezing.
Trigger Shot and Egg Retrieval
When the follicles reach the desired size, a trigger injection is given to prepare the eggs for retrieval. Egg retrieval is a minor outpatient procedure done under sedation or anaesthesia. A thin needle is passed through the vaginal wall using ultrasound guidance to collect the eggs from the ovaries.
This process usually takes less than 30 minutes and is followed by a few hours of rest.
Sperm Collection and Preparation
Sperm is collected from the male partner on the same day as egg retrieval. In some cases, donor sperm or frozen sperm may be used. The sample is washed and processed in the lab to isolate the healthiest, most active sperm.
Fertilization and Embryo Culture
The retrieved eggs are then combined with sperm in the lab. This can happen in two ways:
- Conventional IVF: Eggs and sperm are placed together in a dish and fertilization occurs naturally.
- ICSI: A single sperm is directly injected into each egg, especially useful in cases of poor sperm quality or previous failed fertilization.
Fertilized eggs begin to develop into embryos. These are monitored for 3 to 5 days to assess their growth, appearance, and cell division. The best-quality embryos are selected for transfer or freezing.
Preimplantation Genetic Testing (optional)
If indicated, embryos can be biopsied at the blastocyst stage (Day 5 or 6) to test for chromosomal abnormalities or specific genetic conditions. Only healthy, chromosomally normal embryos are chosen for transfer.
Embryo Transfer
A selected embryo is transferred into the uterus using a soft catheter. This is a simple, usually painless procedure done without anaesthesia. The timing of transfer may vary:
- Fresh Transfer: Embryo is placed in the uterus 3 to 5 days after egg retrieval
- Frozen Transfer (FET): Embryo is thawed and transferred in a later cycle, giving time for the body to recover or for hormone levels to be adjusted
Luteal support (typically progesterone supplements) is given to support implantation and early pregnancy.
Pregnancy Test and Follow-Up
About 10 to 14 days after embryo transfer, a beta hCG blood test is done to confirm pregnancy. If positive, ultrasound scans are scheduled over the next few weeks to monitor the development and confirm heartbeat.
If the result is negative, the next steps are discussed based on remaining embryos, cycle feedback, and emotional readiness. Some people proceed with a frozen transfer; others may revise the treatment plan.
While this is a general outline, ART protocols can be tailored based on individual needs, medical history, and lab findings. No two cycles are exactly the same, and your fertility team will adjust the approach depending on how your body responds.
Success Rates and What Affects Assisted Reproductive Technology (ART) Outcomes
The success of Assisted Reproductive Technology depends on a complex mix of biological, medical, and sometimes lifestyle-related factors. While ART offers powerful solutions for people facing fertility challenges, it’s important to understand that no treatment can guarantee pregnancy. Success is measured by the ability to achieve a healthy pregnancy and live birth, and outcomes can vary widely based on individual circumstances.
Age is one of the most important factors.
The quality and quantity of eggs decline with age, which directly affects embryo viability and implantation potential. ART success rates are generally higher for people under 35 and decrease progressively as age increases. Even when donor eggs are used, the age of the egg donor—not the person carrying the pregnancy—has the strongest impact on success.
Typical success rates by age using IVF with own eggs:
- Under 35: 40–50% per embryo transfer
- 35–37: 30–40%
- 38–40: 20–25%
- 41–42: 10–15%
- Over 43: Less than 10%
If donor eggs are used, success rates often exceed 50–60%, even for people in their 40s, because donor eggs typically come from younger individuals with high ovarian reserve.
Other key factors that influence ART success include:
Egg and sperm quality
Healthier eggs and sperm lead to higher fertilization rates, better embryo development, and improved chances of implantation. This is especially important in cases of advanced maternal age or male factor infertility.
Embryo grading and developmental stage
Embryos are graded based on shape, cell number, and division rate. Transferring high-quality embryos at the blastocyst stage (Day 5) often leads to better success rates than earlier transfers at Day 3.
Uterine receptivity
A healthy endometrial lining, ideally 8–12 mm thick and triple-layered on ultrasound, improves the chances of successful implantation. Some cases may benefit from a mock cycle or endometrial receptivity testing (ERA) to optimise timing.
Cause of infertility
The underlying condition—whether it’s endometriosis, unexplained infertility, male factor, or low ovarian reserve—plays a role in how the body responds to treatment and whether additional support (like ICSI or PGT) is required.
Lifestyle and health factors
Body mass index (BMI), smoking, alcohol use, chronic stress, thyroid dysfunction, and unmanaged medical conditions can negatively impact hormonal balance, egg quality, and uterine environment. These should ideally be addressed before starting ART.
Lab and clinic expertise
Not all fertility clinics have the same success rates. The quality of embryology labs, experience of the fertility team, and adherence to international standards significantly impact outcomes. Always ask for clinic-specific success data before beginning treatment.
Use of advanced technologies
Tools like ICSI (for male factor infertility), PGT-A (for embryo chromosomal testing), time-lapse embryo monitoring, and cryopreservation have improved ART outcomes, especially in complex or repeated failure cases.
Number of cycles attempted
While some people conceive in the first cycle, others may need multiple attempts. Cumulative success rates improve over time, particularly if frozen embryos are available from previous cycles.
Understanding these variables helps set realistic expectations and allows for better planning. It also reminds us that ART is not a one-size-fits-all process—it works best when protocols are adapted to each individual’s biology and clinical history.
Risks and Considerations in Assisted Reproductive Technology (ART)
Assisted Reproductive Technology is generally safe, and millions of successful pregnancies have been achieved using ART worldwide. However, as with any medical intervention, it does come with certain risks and considerations—some physical, others emotional, financial, or ethical.
Understanding these possibilities helps individuals and couples make informed choices, manage expectations, and prepare for the practical realities of treatment.
Ovarian Hyperstimulation Syndrome (OHSS)
In some IVF cycles, the hormone injections used to stimulate egg production can cause the ovaries to over-respond. This can lead to OHSS—a condition where the ovaries become swollen and fluid may accumulate in the abdomen.
Symptoms can include bloating, nausea, weight gain, and abdominal discomfort. Most cases are mild and resolve on their own, but moderate to severe OHSS may require medical monitoring or temporary treatment. Today, newer stimulation protocols and trigger medications have greatly reduced the incidence of serious OHSS.
Multiple Pregnancy
Transferring more than one embryo increases the likelihood of twins or triplets, which can lead to higher risks for both the parent and the babies. These risks may include preterm birth, low birth weight, gestational diabetes, and complications during delivery.
To reduce these risks, many fertility specialists now recommend single embryo transfer (SET), especially for younger individuals or when using genetically screened embryos.
Ectopic Pregnancy
Although rare, there is a small chance that an embryo may implant outside the uterus, usually in the fallopian tube. This is called an ectopic pregnancy and requires immediate medical attention. The risk of ectopic pregnancy in ART is similar to that in natural conception but is closely monitored through early ultrasounds.
Procedure-related risks
Egg retrieval is a minor surgical procedure performed under sedation. While complications are rare, possible risks include infection, bleeding, or injury to nearby organs. Fertility clinics take standard precautions to minimise these risks and provide aftercare guidelines for recovery.
Emotional and Psychological Impact
ART can be emotionally demanding. The anticipation, physical demands of treatment, hormonal changes, and waiting periods can cause anxiety, mood swings, or fatigue. Failed cycles can be particularly distressing.
Support from partners, mental health professionals, or fertility counsellors can be invaluable during this journey. Many clinics also provide access to support groups or one-on-one counselling as part of the treatment process.
Financial Stress
ART can be expensive, especially when multiple cycles, advanced techniques, or donor/surrogacy arrangements are involved. In India, while ART is relatively affordable compared to other countries, the cost is still significant for many families.
Financial counselling, understanding what’s included in treatment packages, and exploring EMI or insurance coverage (if available) can help reduce financial pressure.
Ethical and Legal Considerations
Certain ART procedures, particularly those involving donor gametes or surrogacy, come with ethical and legal implications. In India, ART is governed by the Assisted Reproductive Technology (Regulation) Act and Surrogacy (Regulation) Act, which outline specific eligibility, consent, and documentation requirements.
It’s important to understand and comply with these laws, especially in cases involving third-party reproduction, to avoid legal complications later on.
Long-term Safety
Research continues to track the long-term health of children born through ART. So far, studies show that ART-conceived children are generally as healthy as those born through natural conception. That said, as the technology evolves, ongoing monitoring helps ensure safety across generations.
Being aware of these risks does not mean ART should be feared—but rather, approached with a well-rounded understanding. Proper medical guidance, a personalised protocol, and access to support systems can make the experience smoother, safer, and more empowering.
Cost of Assisted Reproductive Technology (ART) Treatments in India
Assisted Reproductive Technology treatments in India are significantly more affordable than in many other parts of the world, making the country a leading destination for fertility care. However, the cost of ART can still vary widely based on the type of procedure, the clinic’s location and infrastructure, the use of additional technologies, and the patient’s individual medical needs.
Understanding what goes into the cost structure helps patients plan better and avoid unexpected expenses during treatment.
Cost of IVF (In Vitro Fertilization)
A single IVF cycle in India typically ranges from ₹90,000 to ₹2,50,000 depending on the clinic and protocol. This base cost usually includes:
- Initial consultation and fertility scans
- Hormone monitoring during stimulation
- Egg retrieval procedure
- Sperm preparation and fertilization (conventional IVF)
- Embryo culture for 3–5 days
- One fresh embryo transfer
- Basic follow-up and pregnancy test
However, many IVF packages do not include medications, which can add another ₹50,000 to ₹80,000 depending on dosage requirements.
Additional Costs Based on Procedure Type or Complexity
- ICSI (Intracytoplasmic Sperm Injection): ₹20,000 – ₹50,000
- Frozen embryo transfer (FET): ₹30,000 – ₹60,000
- Embryo freezing (vitrification): ₹15,000 – ₹30,000
- Storage of frozen embryos: ₹5,000 – ₹15,000 per year
- Preimplantation Genetic Testing (PGT-A): ₹60,000 – ₹1,50,000
- Donor sperm (if needed): ₹10,000 – ₹25,000
- Donor eggs (if needed): ₹40,000 – ₹1,00,000
- Surrogacy (gestational carrier): ₹10–₹15 lakhs or more, subject to legal and ethical eligibility
Factors That Influence the Overall Cost
- Location of the clinic — metro cities often have higher base rates but offer more advanced labs and techniques
- Patient’s medical profile — lower ovarian reserve or failed past cycles may require higher medication doses or more complex protocols
- Need for additional cycles — success is not guaranteed in one cycle, and costs increase with repeat attempts
- Use of donor programs or advanced lab technology — increases cost but may improve success, especially in difficult cases
Financing and Affordability Options
Most ART procedures in India are not covered by standard health insurance plans, although some newer policies now offer fertility add-ons. Many reputable fertility centers now offer:
- EMI or zero-interest financing options
- Package plans (e.g., two or three IVF cycles bundled)
- Discounted rates for patients opting for multiple treatments
- Transparent billing with no hidden charges
Before beginning treatment, it’s advisable to ask for a written estimate, confirm what is and isn’t included, and check how costs may change based on your response to treatment.
While cost is an important consideration, it should always be weighed alongside clinical quality, lab standards, patient care, and long-term outcomes. Choosing the right fertility team and approach can often save money in the long run by improving the chances of success within fewer cycles.
Assisted Reproductive Technology (ART) vs Other Fertility Treatments
Assisted Reproductive Technology is often seen as the most advanced option in fertility care, but it is not always the first line of treatment. Many individuals or couples begin with simpler, less invasive approaches before moving on to ART procedures like IVF or ICSI.
Understanding how ART compares to other fertility treatments helps clarify where it fits in the broader spectrum of reproductive care.
What’s the difference between ART and non-ART treatments?
The key distinction lies in the level of medical intervention and whether gametes (eggs and sperm) are handled outside the body. Non-ART treatments typically aim to stimulate or support natural conception, whereas ART involves laboratory-based fertilization and embryo transfer.
Common non-ART fertility treatments include:
- Ovulation induction (OI): Medications like clomiphene citrate or letrozole are used to stimulate ovulation in those with irregular cycles. It’s a first-line option, especially for conditions like PCOS.
- Timed intercourse: Tracking ovulation using ultrasound, basal body temperature, or hormone kits to time intercourse for optimal fertility.
- Intrauterine insemination (IUI): Washed sperm is inserted directly into the uterus around the time of ovulation. It is less invasive than IVF and does not involve handling eggs or embryos in a lab.
- Lifestyle modification: Addressing factors like weight, stress, smoking, or thyroid levels can significantly impact fertility and is often combined with other methods.
When is ART recommended instead?
ART is typically advised when:
- Non-ART treatments have failed after several attempts
- There are anatomical issues such as blocked fallopian tubes or severe endometriosis
- There is significant male factor infertility (e.g., low sperm count or motility)
- Fertility preservation is needed (e.g., before cancer treatment)
- Genetic screening is required before pregnancy
- Same-sex couples or single parents are trying to conceive using donor sperm or eggs
- There’s an urgency to conceive, such as in older patients or those with low ovarian reserve
Comparing ART and IUI:
Aspect | IUI | IVF (ART) |
Where fertilization happens | Inside the body | In the lab |
Invasiveness | Less invasive | More invasive |
Success rate per cycle (under 35) | ~10–15% | ~40–50% |
Cost (approx.) | ₹10,000–₹25,000 | ₹1,50,000–₹2,50,000 |
When used | Mild cases, early attempts | Advanced cases, failed IUI, or age factor |
In summary, ART offers the highest level of control and precision, but it’s not always the first step. Your fertility specialist will typically evaluate your case and suggest a treatment path that starts with simpler options unless clinical reasons demand ART from the outset.
Common Questions About Assisted Reproductive Technology (ART)
What does ART actually involve?
ART includes medical procedures where eggs, sperm, or embryos are handled outside the body to assist in conception. It primarily includes IVF, ICSI, embryo freezing, donor programs, and surrogacy.
Is ART the same as IVF?
IVF is a type of ART, but ART also includes other techniques like ICSI, IUI, embryo donation, and surrogacy. So while all IVF is ART, not all ART is IVF.
Who should consider ART?
ART is typically considered when natural conception fails, or when factors like blocked tubes, male infertility, advanced maternal age, or previous treatment failures make conception unlikely without assistance.
Is ART painful?
Most ART procedures are not painful. Hormonal injections may cause mild discomfort, and egg retrieval is performed under sedation. Embryo transfer is usually quick and painless.
What are the chances of success with ART?
Success rates depend on age, egg and sperm quality, medical history, and the type of ART used. IVF success rates range from 40–50% in people under 35 and decrease with age.
Can I use donor sperm or donor eggs with ART?
Yes. ART allows for the use of donor gametes in cases of severe infertility, genetic risks, or for single parents and same-sex couples.
Are ART babies healthy?
Yes. Children born through ART are generally as healthy as those conceived naturally. Ongoing studies continue to confirm this across large populations and age groups.
Does ART guarantee pregnancy?
No fertility treatment can guarantee pregnancy. ART significantly increases the chances, but outcomes depend on many factors including embryo quality, uterine receptivity, and overall health.
Can I work while undergoing ART treatment?
Yes. Most people continue their regular routine during treatment. Some may take a day off around egg retrieval or embryo transfer, but no extended leave is usually required.
How long does an ART cycle take?
A typical IVF cycle takes about 4 to 6 weeks from the start of stimulation to the pregnancy test. Some cases may require more time due to pre-treatment or frozen transfers.
How many ART cycles are usually needed?
Some conceive in one cycle, but others may need two or three. Cumulative success improves with multiple well-managed cycles, especially if frozen embryos are available.
What happens to extra embryos?
High-quality embryos that are not transferred can be frozen for future use. This allows for additional attempts without repeating the entire IVF cycle.
Is there an age limit for ART in India?
According to current Indian guidelines, ART is generally allowed up to age 50 for women and 55 for men, although success declines significantly after age 40.
What is the cost of ART treatment in India?
ART costs vary. IVF usually ranges from ₹90,000 to ₹2.5 lakhs per cycle. Additional costs apply for medications, ICSI, donor gametes, PGT, or embryo freezing.
Can ART be done with virtual consultations?
Yes. Many clinics offer online consultations, pre-treatment counselling, and digital reporting. However, procedures like scans, retrievals, and transfers must be done in person.
Is Assisted Reproductive Technology (ART) Right for You?
Assisted Reproductive Technology has made parenthood possible for millions of people around the world—across different ages, health conditions, and life circumstances. Whether you’re facing a medical diagnosis like low ovarian reserve, struggling with unexplained infertility, or exploring options as a single parent or same-sex couple, ART offers a structured, scientifically supported path to conception.
That said, ART is not for everyone—and it isn’t always the first or only step. The right time to consider ART depends on your age, fertility diagnosis, treatment history, and future plans. For some, it may be the first line of care; for others, it may follow after trying simpler treatments like ovulation induction or IUI.
A fertility consultation is the best way to understand what’s right for you. With the help of diagnostic tests, expert review, and a personalised care plan, you can make informed decisions that align with your goals, your body, and your timeline.
If you’re thinking about ART, here are a few good starting points:
- Book a fertility consultation with a qualified specialist
- Explore whether IVF, ICSI, or another ART method may be appropriate
- Use online tools like fertility timelines or success rate calculators
- Ask about package pricing, second opinions, or digital consultations
- Read up on success stories and patient experiences
Assisted Reproductive Technology is more than a set of procedures—it’s a gateway to reproductive possibility. With the right guidance and support, it could be the next step in your journey to parenthood